Over the past twenty years, researchers have discovered that the immune system plays a much more significant role in the body than just protecting it from infectious diseases. But it can become damaged as a result of many things, including infections, radiation therapy, transplants, and trauma. When the immune system is down, it can lead to several kinds of disorders:
- Autoimmune diseases: These occur when the immune system is no longer ale to differentiate between proteins that are “self” and “non-self,” and thus begins to attack the body itself.
- Allergies: When the body is exposed to allergens, it has an increased production of IgE immunoglobins, which produces a more severe inflammatory response.
- Acquired immune deficiency disorder (AIDS): When parts of the immune system, mostly T helper cells, disappear or become damaged. This occurs mostly as a result of infection with harmful viruses.
- Immune complex disease: This occurs when antigen-antibody complexes build up and can’t escape the body’s tissues, which ultimately destroys the organs nearby
- Common variable immunodeficiency (CVID): This is a condition that involves multiple autoimmune disorders at once, which might include inflammatory bowel disease (IBD), autoimmune thrombocytopenia, and autoimmune thyroid disease
- Cancer: The most significant and potentially fatal consequence. So what’s the connection between cancer and the immune system?
 Studies have shown that the immune system is essential in forming tumor immunogenicity, or the body’s ability to induce adaptive immune responses against cancerous tumors. Although the immune system is designed to help fight cancer, unfortunately, the disease oftentimes has ways of evading the immune system’s detection. This process is known as cancer immunoediting, and it consists of three phases, elimination, equilibrium, and escape.
Studies have shown that the immune system is essential in forming tumor immunogenicity, or the body’s ability to induce adaptive immune responses against cancerous tumors. Although the immune system is designed to help fight cancer, unfortunately, the disease oftentimes has ways of evading the immune system’s detection. This process is known as cancer immunoediting, and it consists of three phases, elimination, equilibrium, and escape.
- Phase One – Elimination
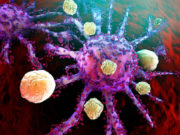
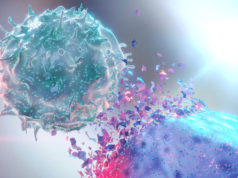
The first phase of immunoediting, also known as cancer immunosurveillance, involves a group of innate and adaptive immune responses that immune cells give off towards the collection of cells that are most likely to create a tumor. When normal cells become tumor cells, some of the antigens on their surface are altered and become absorbed into the bloodstream. Because most of these cells are tumor antigens, the innate immune system responds by sending out inflammatory signals. Then, Natural Killer (NK) cells, NK T lymphocytes, macrophages, and dendritic cells begin to penetrate the tumor cells. They surround the affected cells and produce cytokines, killing off many of the tumor cells as well as stopping the growth of future ones. They inhibit the blood vessels that are responsible for providing nutrients to the tumor cells, which allows them to stop the tumor cells from developing. This process ultimately creates an ongoing death of these cells.
This process continues as the chemokines flowing throughout the body stimulate more immune cells, resulting in the removal of tumor cells from the body. Numerous studies have highlighted the role that NK cells play in tumor immunosurveillance, showing that the multiple receptors found on the surfaces of these cells are integral in identifying antigens and tumor specific proteins that are loose in the bloodstream. Studies performed on mice with NK cells have also shown that there is a greater chance of tumor cells forming in those who have a lower number of NK cells. Both of these studies show how significant NK cytotoxic cells are, above all other parts of the immune system, in the process of tumor immunosurveillance.
- Phase Two – Equilibrium
Although the immune system tries hard to keep an eye on the growth of tumor cells, many cells unfortunately evade the body’s inspection mechanisms and they thus proceed to the equilibrium stage. Their innate characteristics are supposedly immunogenic, and they grow in this phase for a few years, making this phase the longest of the three. It is suggested that the Darwinian concept of natural selection works in the emerging tumor cells so that ultimately the ones that are most likely to fight against the immune system are the ones that survive. This is largely because of their abnormal growth pattern, which contributes to the cell mutations that have developed over time, helping the cells to thrive within the cytotoxic cells of the body.
- Phase Three – Escape
The last phase of immunoediting, during which the mutated tumor cells continue to grow and attack the body’s immune system using many different methods that ultimately cause malignancies and cancer.

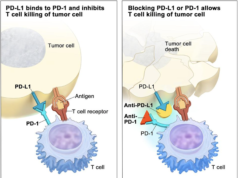
Recent studies in the field of immunotherapy have discovered treatments that work to outsmart cancerous cells and get the immune system to do its job of warding off foreign invaders. This is why immunotherapy has been so successful in treating many different cancers, as it activates the body’s own powerful ability to fight disease.


















Great article.