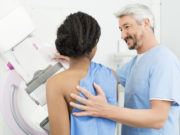
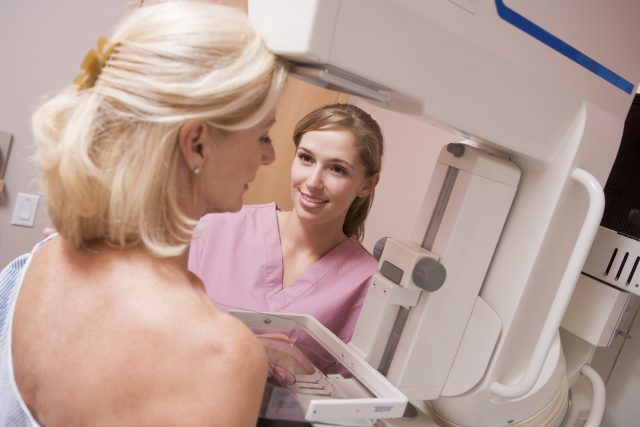
A study sponsored by the charity Breast Cancer Now revealed that women with a family history of breast cancer should start annual screenings in their mid-thirties. Doing so could detect tumors early, prevent the cancer from advancing, and save lives.
Although current guidelines say that women at higher risk for breast cancer begin screenings at age 40, breast cancer is still the leading cause of death in women under 50. It’s essential for clinicians to identify high-risk women and offer them mammograms earlier on.
 The study, which was performed by the University of Manchester, provided mammograms to 2,899 ages 35-39 who were deemed moderate to high risk. These screenings found 35 invasive breast tumors, and may were detected before they traveled to the lymph nodes or the rest of the body. In a control group of patients who did not get screened, many cancers were found to be at later stages that had already spread to the lymphatic system.
The study, which was performed by the University of Manchester, provided mammograms to 2,899 ages 35-39 who were deemed moderate to high risk. These screenings found 35 invasive breast tumors, and may were detected before they traveled to the lymph nodes or the rest of the body. In a control group of patients who did not get screened, many cancers were found to be at later stages that had already spread to the lymphatic system.
 Dr. Gareth Evans, lead author of the study, believes that these results show that annual mammograms are able to detect tumor earlier in younger patients. Baroness Morgan called the study an “enormous breakthrough” that could prevent many lives from being cut “heartbreakingly short.” Identifying and removing these tumors when they are small and haven’t yet spread is a good way to prevent the cancer from ever returning.
Dr. Gareth Evans, lead author of the study, believes that these results show that annual mammograms are able to detect tumor earlier in younger patients. Baroness Morgan called the study an “enormous breakthrough” that could prevent many lives from being cut “heartbreakingly short.” Identifying and removing these tumors when they are small and haven’t yet spread is a good way to prevent the cancer from ever returning.
Researchers believe that if the age guidelines for mammograms changed, it could impact the lives of over 86,000 women. Because between 5 and 15 percent of breast cancers are related to family history, clinicians can confidently identify it as a risk factor in young women.
 It seems as though these results should automatically signal earlier screenings, but it’s not that simple. Aside from the financial burden involved in increased screenings, many professionals say there are actually risks of conducting earlier mammograms. As much as these screenings will pick up earlier incidents of breast cancer, they can also pick up several false positives, which can lead to unnecessary tests and procedures. They also could lead to “over-diagnoses,” when doctors detect and treat cancers that may never have developed into anything.
It seems as though these results should automatically signal earlier screenings, but it’s not that simple. Aside from the financial burden involved in increased screenings, many professionals say there are actually risks of conducting earlier mammograms. As much as these screenings will pick up earlier incidents of breast cancer, they can also pick up several false positives, which can lead to unnecessary tests and procedures. They also could lead to “over-diagnoses,” when doctors detect and treat cancers that may never have developed into anything.
The “risks” of increased screening likely outweigh the benefits, but making definitive changes to the current guidelines will have to be further considered. Officials say that these changes to the screening program in England will be considered in a future review. Breast cancer survival is currently higher than its ever been, and increasing screening methods could be a way to prevent even more people from